Two nights of bad sleep can flip a molecular switch in the brain that looks uncomfortably like the beginning of long-term memory trouble.
Story Snapshot
- A key brain-protective protein in the hippocampus drops after sleep loss, and that decline lines up with neuron damage and weaker memory performance.
- Large human imaging datasets tie “too little” or “too much” sleep to subtle brain injury markers linked with stroke and dementia risk.
- Midlife sleep problems don’t just make you foggy; they correlate with measurable brain-aging patterns over time.
- The newest lab work suggests attention lapses during sleep deprivation may involve brain fluid dynamics, not only willpower or “toughness.”
The PTN clue: why “just power through” fails as a brain strategy
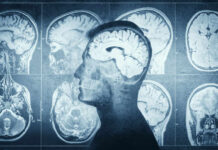
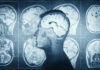
Researchers sleep-deprived mice for two days, then tested them on maze navigation and object recognition—classic ways to measure hippocampus-based memory. The animals performed worse, but the bigger shock came from the protein mapping of the hippocampus. Levels of pleiotrophin (PTN), a neuroprotective protein, dropped. Lower PTN tracked with neuronal death and cognitive impairment, making sleep loss look less like a mood problem and more like a biological injury problem.
PTN matters because it offers a concrete “handle” on what sleep protects. A lot of sleep advice sounds like lifestyle nagging until you can point to a molecule that supports neuron survival in the region that helps you form new memories. The study’s extra step—connecting the mouse findings through systems genetics to human neurodegenerative signals—raises the stakes: the same direction of risk shows up where Alzheimer’s disease lives, even if mice are not people.
One bad night versus chronic deprivation: the brain keeps receipts
People who treat sleep like a negotiable expense usually measure consequences in coffee cups: more caffeine, more grit, more “I’m fine.” Biology measures it differently. Even a single night of sleep loss has been associated in prior work with changes tied to beta-amyloid, the substance linked with Alzheimer’s plaques. Over time, chronic short or fragmented sleep disrupts the normal NREM/REM rhythm that supports memory consolidation, and the cost can show up as false memories, rigid thinking, and emotional misfires.
Midlife is the danger zone because it combines peak responsibility with quiet accumulation of damage. The research focus on adults roughly 40 to 69 isn’t arbitrary; it reflects a window where risks become measurable but interventions still have time to pay off. That framing aligns with common sense: you can’t reverse every mile on the odometer, but you can stop driving with the oil light on. Sleep is closer to maintenance than luxury, and the brain acts accordingly.
What big population brain scans say about “suboptimal” sleep
Mechanisms feel abstract until the MRI data arrives. A large neuroimaging analysis drawing from UK Biobank scans linked suboptimal sleep—less than seven hours or nine hours and up—to markers associated with poorer brain health, including white matter hyperintensities and reduced fractional anisotropy. Those findings matter because they sit upstream of clinical events: stroke, cognitive decline, dementia. The study also attempted to adjust for common confounders, strengthening the argument that sleep itself plays a meaningful role.
The useful takeaway is practical and individual. Sleep sits in the same modifiable-risk bucket as weight control, blood pressure, and exercise—factors that reward personal responsibility and consistent habits. The caution is equally straightforward: “I’ll catch up on the weekend” sounds thrifty, but the brain appears to treat irregular sleep like irregular maintenance.
Midlife insomnia patterns and the “older brain” signature
Another set of findings followed sleep patterns over years and connected persistent trouble—difficulty falling asleep, waking early—to faster brain aging signals on scans. The estimated difference, roughly 1.6 to 2.6 years of accelerated brain aging, lands like a gut punch because it translates insomnia into time you can picture. It doesn’t prove every case is causal, but it does make sleep a credible early intervention target for preserving cognitive function.
That’s the open loop many people miss: you don’t have to wait for obvious memory problems to take sleep seriously. Brain change can be quiet for a long time, then loud all at once. Family history, stress, late-night screens, shift work—these all stack the deck. The sanest response isn’t panic or pills-by-default; it’s treating sleep as a non-negotiable health input, then using medical evaluation when patterns persist.
The weird new twist: attention lapses and brain fluid “flushing”
MIT researchers added a newer layer to the story by tying sleep deprivation to cerebrospinal fluid dynamics during attention lapses. People think of fatigue as heavy eyelids, but the lab angle suggests something more mechanical: the brain’s internal environment may shift during moments when attention drops, helping explain slowed responses and microsleeps. That doesn’t excuse dangerous choices like drowsy driving; it underlines why “I felt fine” is not a reliable safety standard.
The broad theme across these studies is uncomfortable but empowering: sleep loss doesn’t merely reduce your performance; it can alter brain biology in ways that resemble pathways involved in neurodegeneration. Protect sleep the way you protect your retirement account—steady contributions, fewer late withdrawals, and no pretending that tomorrow’s you will magically cover today’s deficit.
Small wins beat heroic bursts: consistent bed and wake times, morning light, fewer late alcohol “nightcaps,” and treating snoring or insomnia as medical issues rather than personality quirks. The research doesn’t demand perfection; it suggests thresholds. If seven to nine hours is the stable middle and extremes correlate with risk markers, aim for the boring center. Boring is underrated when the payoff is keeping your memory sharp.
Sources:
How Sleep Deprivation Can Harm the Brain
Lack of Sleep and Cognitive Impairment
Poor sleep may increase markers of poor brain health, new study finds
Poor Sleep in Midlife Linked to Faster Brain Atrophy
Sleep Health Education Program