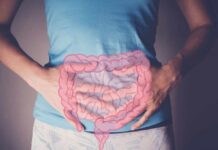
The fries and soda your teenager craves might be doing more damage than you think, rewiring their developing brain in ways that stretch far beyond the bathroom scale.
Story Snapshot
- A 2026 systematic review of 19 studies found healthier dietary patterns consistently reduced depressive symptoms in teens, while vitamin supplements showed weak or inconsistent results.
- Adolescence represents a critical brain development window where ultra-processed foods, sugars, and fast food correlate with psychological distress, while fruits, vegetables, and whole grains support mental health.
- Professor Hayley Young from Swansea University advocates prioritizing whole-diet approaches over supplements for scalable public health interventions targeting teen mental wellness.
- Socioeconomic status and sex confound many findings, with girls and low-income teens at heightened risk for diet-related mental health challenges.
- Researchers propose a roadmap for future studies using biological markers and standardized methods to establish causal links, addressing gaps in anxiety and behavioral outcomes.
The Research That Changes Everything for Teenage Mental Health
Swansea University researchers published a groundbreaking systematic review in Nutrients during early 2026, synthesizing evidence from six randomized controlled trials and 13 cohort studies involving adolescents. The findings revealed a consistent inverse relationship between diet quality and depressive symptoms. Teens consuming diets rich in fruits, vegetables, and whole grains while limiting ultra-processed foods showed fewer mental health struggles. This marked the first comprehensive adolescent-specific synthesis, distinguishing itself from decades of adult-focused nutrition psychiatry research that examined Mediterranean diets and depression.
The review exposed a critical gap: while vitamin D and omega-3 supplements dominated clinical trials, their effects remained inconsistent or weak. Professor Young emphasized public health strategies should abandon the supplement fixation and instead promote accessible dietary patterns. The research team proposed standardized exposure studies incorporating biological markers to move beyond observational associations. This approach addresses adolescence as a unique developmental stage, when emotion and reward brain regions undergo rapid rewiring that demands specific micronutrients for optimal function.
Why Your Teen’s Brain Demands Better Fuel
Adolescence spans ages 10 to 19, a period marked by profound neurological changes in regions governing emotional regulation and impulse control. During these years, erratic eating habits flourish, junk food consumption spikes, and nutritional vulnerabilities intensify. Western dietary patterns characterized by high sugar, saturated fat, and processed foods create a toxic environment for developing neural pathways. The brain’s plasticity during this window makes it particularly susceptible to dietary influences, amplifying both the risks of poor nutrition and the potential benefits of intervention.
Studies included in the review demonstrated that perceived healthy eating correlated with improved stress management skills among 505 urban school teens. This connection strengthened when peer support systems reinforced positive dietary choices. Girls and students repeating grades faced disproportionate risks, suggesting socioeconomic factors and academic stressors compound nutritional effects on mental health. The interplay between diet, social context, and brain development creates a complex web that simple supplement regimens cannot address, explaining why whole-diet interventions show more promise.
The Uncomfortable Truth About Supplements and Quick Fixes
Parents seeking easy solutions through vitamin bottles will find little comfort in this evidence. The supplement industry has long promoted vitamin D and omega-3 fatty acids as mental health panaceas, yet the adolescent data tells a different story. Trials testing these isolated nutrients produced inconsistent results, with many studies showing no significant impact on depressive symptoms once researchers controlled for confounding variables like family income and baseline activity levels. This pattern suggests nutrient interactions within whole foods deliver benefits that manufactured pills cannot replicate.
The IAFNS-funded review authors noted that associations between diet and mental health often weakened when accounting for socioeconomic status and behavioral factors. This finding aligns with common sense: families with resources to purchase fresh produce likely benefit from multiple protective factors beyond nutrition alone. Yet even after statistical adjustments, healthier dietary patterns maintained significant associations with better mental health outcomes. The Mediterranean diet showed particular promise despite limited adolescent-specific data, pointing toward a need for culturally adapted, whole-food approaches rather than one-size-fits-all supplement protocols.
What Parents and Policymakers Should Do Now
Short-term implications suggest clinicians and public health officials should pivot toward dietary counseling for at-risk adolescents rather than defaulting to supplement recommendations. Targeting interventions at low-income teens and girls addresses populations facing compounded vulnerabilities. Schools represent ideal intervention points, where nutrition education and improved meal programs could reach adolescents during their most malleable developmental phase. The scalability of whole-diet approaches surpasses medical interventions, offering prevention strategies accessible across socioeconomic boundaries without requiring clinical infrastructure.
What teens eat could be affecting their mental health more than we thought – https://t.co/lJWbTR33uX
— Ken Gusler (@kgusler) March 29, 2026
Long-term impacts could reshape how society approaches adolescent mental health prevention. Reducing lifelong depression and metabolic disease burdens through teenage nutrition interventions makes fiscal sense, potentially lowering healthcare costs compared to pharmaceutical treatments. The food industry faces pressure to reduce ultra-processed product marketing to teens, while policymakers may incorporate nutrition guidelines into youth mental health frameworks. However, evidence gaps around causality, anxiety outcomes, and high-risk populations limit immediate policy adoption. Professor Young’s proposed research roadmap using biomarkers and rigorous randomized trials aims to fill these gaps, building the evidence base needed for confident public health action.
Sources:
Healthy dietary patterns linked to better adolescent mental health
Diet and adolescent mental health prevention
Effects of diet on teen mental health need closer study
Optimizing mental health through nutrition during adolescence
Teen diet mental health review
Vitamin D shows inconsistent effects but dietary strategy could improve teens mental health
Research on the link between nutrition stress and teen mental health