One in three women taking hormonal therapy for endometriosis watch their pain return within two years, despite following doctor’s orders perfectly.
Story Snapshot
- Medical treatments fail to reduce pain in 11 to 19 percent of women initially, with recurrence rates hitting 17 to 34 percent after stopping therapy
- Forty-three percent of women receiving hormonal therapy report no improvement, while only 17 percent feel satisfied after surgery
- The average endometriosis diagnosis takes seven to nine years as doctors dismiss symptoms as normal period pain
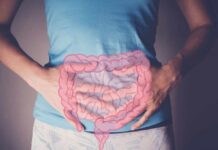
- No cure exists for the 190 million women worldwide suffering from tissue growing outside the uterus, causing chronic pelvic pain and infertility
The Treatment Paradox That Medicine Won’t Acknowledge
Clinical trials paint an optimistic picture of endometriosis treatment, reporting discontinuation rates of just 5 to 16 percent. Real-world data tells a starkly different story. Women abandon treatments at rates of 15.6 to 43.5 percent, fleeing either crushing side effects or complete ineffectiveness. A 2017 systematic review analyzing 58 studies across four decades revealed this gap between laboratory success and lived failure. The disconnect raises uncomfortable questions about whether pharmaceutical companies and researchers are measuring what matters to the women enduring this disease.
The numbers get worse when you look beyond the initial prescription. Between 5 and 59 percent of women remain symptomatic even while actively taking medication. Pain scores drop during treatment, then rebound within six months of stopping. This yo-yo effect traps women in a cycle of temporary relief followed by relapse, with each iteration eroding hope and trust in the medical system. Progestins, the current first-line defense, leave 27 to 34 percent of women dissatisfied, a figure that should alarm anyone claiming current treatments are adequate.
When Your Brain Amplifies Pain Medicine Can’t Touch
Surgery was supposed to be the answer when hormones failed. Remove the misplaced tissue, eliminate the source, end the pain. Except it doesn’t work that way for everyone. Brain imaging studies now show that some women develop central sensitization, where the nervous system itself becomes hyperactive, amplifying pain signals even after surgeons remove every visible lesion. This neurological shift explains why cutting out endometriosis tissue brings relief to some while leaving others in agony. The medical establishment has been performing the same procedures for decades without accounting for this fundamental difference in how chronic pain operates.
UK National Health Service data exposes the scope of this oversight. Doctors prescribe hormonal therapy to 77.9 percent of diagnosed women, yet refer only 7.4 percent to pain specialists. Instead, 8.7 percent receive gabapentinoids, medications with zero evidence of effectiveness for endometriosis pain. This scattershot approach to pain management reveals a system more comfortable following treatment algorithms than addressing the complex reality of individual patient response. When standard treatments fail, women face either ineffective medications or the opioid pathway with its attendant addiction risks.
The Seven Year Wait Before Anyone Believes You
Endometriosis affects one in ten reproductive-age women, yet the average time from first symptoms to diagnosis stretches seven to nine years. During that lost decade, tissue continues growing, pain intensifies, and fertility windows narrow. The delay stems from a pernicious dismissal of women’s pain as normal menstruation, a cultural and medical failure with concrete consequences. By the time doctors take symptoms seriously, the disease has often progressed to stages requiring more aggressive intervention. This diagnostic negligence particularly harms women seeking to preserve fertility, as treatment delays compound reproductive challenges.
The research funding gap perpetuates this crisis. Endometriosis receives a fraction of the research dollars allocated to conditions affecting similar population sizes, leaving treatment options stuck in a decades-old paradigm of symptom suppression rather than cure. Hormonal therapies dating to the 1970s and 1980s remain the standard approach, offering 40 to 70 percent of women short-term relief while providing no path to permanent resolution. The World Health Organization acknowledges limited access to adequate care persists globally, yet breakthrough treatments remain confined to theoretical future development rather than current clinical practice.
What Comes Next When Nothing Works
Emerging approaches focus on non-hormonal pain management and fertility preservation, acknowledging that one-size-fits-all treatment fails too many women. Researchers are exploring how brain imaging might identify which patients will respond to lesion removal versus those requiring neurological pain interventions. This personalized approach makes intuitive sense, though it requires abandoning the comfortable fiction that current protocols work for everyone. The question remains whether medical institutions and pharmaceutical companies will invest in solutions for the 17 to 34 percent of treatment failures or continue optimizing therapies that already succeed for the majority.
Cost-effectiveness analysis suggests surgery becomes economically justified after three failed medication trials, yet this calculus ignores years of diminished quality of life while women cycle through ineffective hormonal therapies. The approach of exhausting pharmaceutical options before surgical referral may protect healthcare budgets, but it extends suffering for women whose physiology doesn’t respond to hormone suppression. A system that genuinely prioritized patient outcomes would accelerate access to multidisciplinary pain specialists and surgical evaluation rather than forcing women through predictable treatment failures. Until research funding, diagnostic urgency, and treatment individualization match the scale of this disease, endometriosis will continue failing women at rates that should be unacceptable to any healthcare system claiming to serve them.
Sources:
Response and Failure of Medical Treatment of Endometriosis
Reevaluating Response and Failure of Medical Treatment of Endometriosis
UK NHS Endometriosis Treatment Patterns and Satisfaction
Endometriosis: Diagnosis and Management
How Common Treatments for Endometriosis Are Failing Those With Chronic Pain